Items filtered by date: December 2023
Causes and Treatment of Toenail Fungus
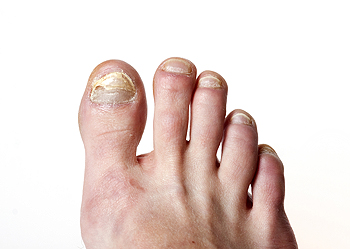
Toenail fungus, or onychomycosis, affects up to 14 percent of the population, with a higher incidence in toenails. Symptoms include discoloration, thickening, brittleness, and nail distortion. Advanced cases of toenail fungus may involve nail detachment, causing pain and potential infections. Fungal nail infections result from exposure to environmental fungi, exploiting small cracks in nails or surrounding skin. Risk factors include nail injuries, foot deformities, and trauma, creating entry points for fungi. Diabetes increases susceptibility due to compromised circulation and weakened immunity. Cancer or conditions suppressing the immune system elevate vulnerability. Poor leg circulation, such as venous insufficiency, or narrowed arteries, signaling peripheral artery disease, can contribute to the susceptibility for fungal nail infections. Those with a history of fungal skin infections are also more prone, especially anyone with a weakened immune system. Secondary bacterial infections are common in people with diabetes, amplifying health risks. Understanding toenail fungus causes and symptoms is essential for early detection. If you believe you have developed a toenail fungus infection, it is suggested that you schedule an appointment with a podiatrist who has advanced measures that can help rid you of this stubborn condition.
For more information about treatment, contact one of our podiatrists of Parkwood Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our offices located in Brunswick and Hinesville, GA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Causes and Symptoms of Foot Stress Fractures
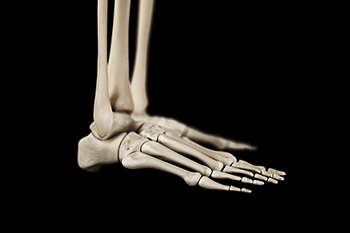
Foot stress fractures, prevalent among runners, are primarily attributed to overuse, constituting 80 percent of cases. The repetitive forces during running may cause microscopic bone damage, escalating into hairline fractures if adequate recovery time is not provided. Sudden increases in running volume, intensity, or frequency, common in the overtraining syndrome, can make it worse. Running form also plays a role, especially with those who have a pronounced heel strike. However, transitioning abruptly to a forefoot strike or wearing minimal footwear can similarly increase the risk of metatarsal stress fractures. Nutrition is a vital factor in preventing stress fractures of the feet. Low vitamin D levels, specifically during winter, elevate the risk of stress fractures. Runners, especially women, face heightened risk if conditions such as osteoporosis or menstrual cycle-related amenorrhea are present. Additionally, sudden changes in running surfaces, such as switching from trails to roads without proper training, can elevate the risk. Wearing proper footwear is equally as important. Old, ill-fitting shoes that lack proper support can increase bone stress. Balancing training intensity, adopting gradual changes in running techniques, maintaining a nutritious diet, and ensuring proper footwear are key components of a comprehensive approach to foot health and injury prevention. For help in managing foot stress fractures, it is suggested that you schedule an appointment with a podiatrist.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact one of our podiatrists from Parkwood Podiatry. Our doctors can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our offices located in Brunswick and Hinesville, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Common Advice From Podiatrists
Taking an average of 8,000 steps a day, it is essential to give your feet the care they deserve. Podiatrists emphasize the importance of foot health, offering useful advice. One key recommendation is to refrain from walking barefoot in public showers, as they are hotspots for athlete's foot-causing fungus. Wearing protective footwear such as flip-flops or water shoes is advised. Extra attention should be paid to drying the feet, particularly between toes. The condition of your feet can be indicative of overall health. For instance, changes like the disappearance of toe hair or alterations in skin texture may signal peripheral arterial disease, or PAD, which can suggest broader cardiovascular issues. Dry skin and non-healing ulcers could point to undiagnosed diabetes. Choosing the right footwear is critical. Pointy pumps, for example, can lead to bunions and other painful conditions. Shoes with a wide toe box and heels under two inches are recommended. Additionally, the length of your toes matters. If your second toe is longer than your first, it can lead to various foot problems, including bunions and back issues. This condition, known as Morton's toe, requires wearing appropriate footwear to mitigate problems. Toenail fungus is another common issue, often indicated by discolored or brittle nails. Keeping the feet dry and changing sweaty socks frequently may help to avoid fungus. If you would like to obtain additional information about good foot care,it is suggested that you schedule an appointment with a podiatrist who can provide you with useful advice.
If you are experiencing pain in the feet or ankles, don’t join the stubborn majority refusing treatment. Feel free to contact one of our podiatrists from Parkwood Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
Someone would seek the care of a podiatrist if they have suffered a foot injury or have common foot ailments such as heal spurs, bunions, arch problems, deformities, ingrown toenails, corns, foot and ankle problems, etc.
Podiatric Treatment
A podiatrist will treat the problematic areas of the feet, ankle or lower leg by prescribing the following:
- Physical therapy
- Drugs
- Orthotic inserts or soles
- Surgery on lower extremity fractures
A common podiatric procedure a podiatrist will use is a scanner or force plate which will allow the podiatrist to know the designs of orthotics. Patients are then told to follow a series of tasks to complete the treatment. The computer will scan the foot a see which areas show weight distribution and pressure points. The podiatrist will read the analysis and then determine which treatment plans are available.
If you have any questions please feel free to contact our offices located in Brunswick and Hinesville, GA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Arthritis Can Cause Pain in the Feet and Ankles
Exploring the Causes of Cracked Heels
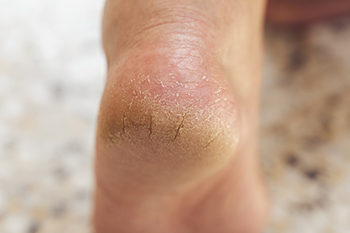
Cracked heels, a common foot ailment, result from a combination of environmental, lifestyle, and health factors. Insufficient moisture is a primary culprit, as dry skin lacks the flexibility to withstand the pressures of daily activities, leading to heel fissures. Prolonged standing or walking on hard surfaces can contribute to the development of cracks, especially when combined with ill-fitting shoes that fail to provide adequate support. Skin conditions such as eczema or psoriasis may exacerbate heel dryness, making them more susceptible to cracking. Unhealthy lifestyle habits, including poor nutrition and dehydration, can impact skin health, diminishing its ability to retain moisture. Obesity or excess body weight increases pressure on the heels, further predisposing them to crack. Additionally, age-related factors such as reduced oil production and diminished skin elasticity make older individuals more prone to cracked heels. If you have developed cracked heels, it is strongly suggested that you visit a podiatrist who can provide you with treatment options, which may include prescribed medication.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact one of our podiatrists from Parkwood Podiatry. Our doctors can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our offices located in Brunswick and Hinesville, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.